Rapid Action Drug Alerts and Response (RADAR) Alerts
Xylazine alert
- Version
- Xylazine alert Show version history
- Published
- 09 May 2024 (Latest release)
- Type
- Guidance
Public health alert: Xylazine – newly detected drug
- Alert area
Scotland
- Action required by
people working and volunteering in drug and alcohol services, emergency services, healthcare and medical settings, and high-risk settings such as prisons and hostels.
- Action required
provide harm reduction interventions for xylazine and polydrug use – see sections marked for specific actions.
- Alert number
2024/09
- Version number
1.0
- Release date
9 May 2024
- Valid until
9 May 2025
Printable summaries of this alert
One-minute summary
Xylazine is a non-opioid tranquiliser used in veterinary medicine as a sedative, muscle relaxant and painkiller. It has been detected in overdoses and deaths in Scotland.
People who take drugs may not be aware of the potential presence of xylazine in the supply. It is most likely to be consumed unintentionally and is usually found as an adulterant in brown powders sold as heroin.
In the UK, it has also been detected in the wider drug supply, including in counterfeit opioid painkillers (codeine and tramadol) and in liquids sold as tetrahydrocannabinol (THC) vapes.
Xylazine is a central nervous system depressant. It reduces breathing, heart rate and blood pressure. Other adverse effects include: sudden collapse, unconsciousness, drowsiness, confusion, loss of coordination, memory loss and nausea.
Xylazine use is associated with the development of severe wounds and skin damage, regardless of how it is administered. The highest risk of wound damage is seen among people who inject drugs. Wounds can appear as spots, blisters or open sores anywhere on the body, and may need medical attention.
As with other new synthetic drugs, the harms associated with xylazine should be considered in the context of polysubstance use (mixing drugs), where the risk of adverse effects is significantly increased.
Xylazine
Xylazine is a depressant that can cause drowsiness, low heart rate and low blood pressure. It is an alpha-2-adrenoceptor (a2) agonist. It binds to a2 receptors in the body causing a reduction in noradrenaline and dopamine, resulting in sedation.
Xylazine can be smoked, snorted, swallowed or injected. It is absorbed, metabolised and eliminated rapidly from the body. Depending on the dose, route of administration, and combination with other substances, the effects of xylazine may begin within minutes and last for eight or more hours.
It is often found as an addition or adulterant to opioids, particularly heroin. Mixing xylazine with other depressants (such as opioids, gabapentinoids, alcohol or benzodiazepines) significantly increases the risk of a life-threatening overdose.
Reports to RADAR describe xylazine as having sleep-inducing and sedative effects. Several reports describe sudden collapse, unconsciousness and memory loss. In addition, it is reported to be associated with the development of severe wounds and skin ulcers.
- wounds and tissue necrosis (skin death)
- sudden collapse
- unconsciousness (will not wake when shaken)
- drowsiness
- confusion
- relaxation
- euphoria
- memory loss and blackouts
- headaches
- vomiting
- reduced coordination
- reduced heart rate
- reduced response
- slurred speech
- high blood sugar
Detections
This alert applies to all of Scotland. There have been detections of xylazine in most NHS boards.
The first known detection in Scotland was in January 2020 by WEDINOS. There were a small number in 2022, but detections increased quickly in the second half of 2023.
Xylazine was present in samples from:
• 13 overdoses (ASSIST emergency department attendances, Glasgow, July 2023 to February 2024)
• 8 deaths (post-mortem toxicology, national, July to December 2023).
In all 21 samples, it was detected alongside other drugs, most commonly heroin, bromazolam, codeine, metonitazene, protonitazene and cocaine.
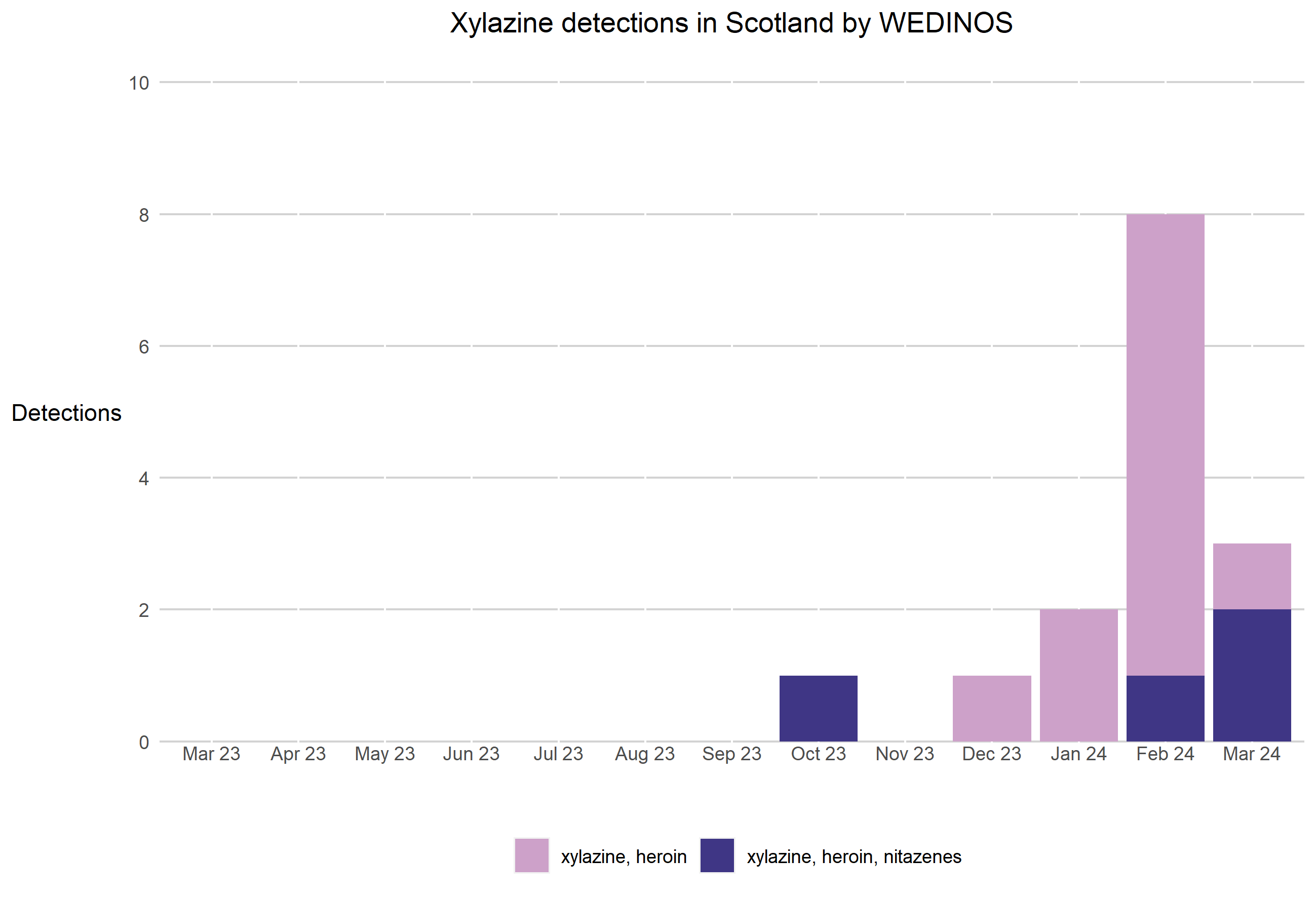
Source: WEDINOS public data for self-selecting samples – www.wedinos.org/sample-results (external website)
Between 1 October 2023 and 31 March 2024, WEDINOS detected xylazine in 15 samples sent from Scotland (Lothian, Borders, Forth Valley):
- 53% (8) were described as a powder and 47% (7) were a solid.
- 53% (8) were brown and the rest were described as pink, green/brown, red/brown, pink/grey, black/brown or grey/brown.
- 100% (15) were purchased as heroin. All contained at least morphine/heroin and xylazine. Three also contained metonitazene and one contained metonitazene, protonitazene, bromazolam and nitrazolam.
- Xylazine was detected in 75% of all Scottish ‘heroin’ samples submitted to WEDINOS (15 of 20). Note: This may not be representative of the wider market as people may be more likely to send in samples they are concerned about.



Wound care
The mechanism by which xylazine causes wound damage is not well understood. Xylazine can cause blood vessels to narrow and reduce the blood supply to the skin which can slow down healing of wounds and increase the chance of skin ulceration, infections and other complications.
People who inject drugs are at the highest risk of harm due to the direct toxic effect of xylazine on the skin, patterns of injection and toxicity of other substances which may be injected at the same time.
Wounds may appear as bruises, spots, blisters, ulcers and black lesions. They are most likely to occur at administration sites but can occur anywhere on the body, including the forearms and lower legs.
First aid should be carried out where necessary. Specific wound care interventions should be provided by trained staff.
Reduce the risks of infection
- Avoid injecting. This route of administration poses the highest risk. If you do inject, use new equipment. You can get this from your local needle exchange service.
- Try to find a safe clean space and wipe down surfaces before preparing drugs.
- Wash your hands and injection sites (before and after).
- Maintain good hygiene and keep wounds clean. Washing with warm water is appropriate for most wounds. Alcohol swabs should not be used.
- Seek prompt medical care for wounds and injuries. A simple dressing should be applied until medical care and assessment can take place.
Recognise infection
- Signs of infection include:
- heat, redness or swelling around the wound that is getting worse
- more yellow, green or black in the wound than before
- wetter
- more painful
- bigger or deeper
- bad smell.
- Infections can be life-threatening. They can spread to affect the entire body and you can become seriously unwell very quickly.
- Early intervention can prevent further harm and injury. If there are signs of infection, get medical help. Call 111 for advice. Needle exchanges, GPs, minor injury clinics and pharmacies may also be able to help. In an emergency, visit the emergency department.
Any increase in wound-related presentations or bacterial infections, such as invasive group A strep (iGAS), can be reported to NHS Health Protection Teams.
Resources
Further advice for workers and people who use drugs is available from the Scottish Drugs Forum (SDF):
Recognising and responding to an overdose
Depressant drug overdose signs
- unresponsive (will not wake when shaken)
- snoring or noisy breathing
- seizures or fits
- nausea and vomiting
- blue or pale lips and skin
- pin-point pupils (sign of opioid use)
People may be taking a combination of drugs with different effects and the signs may not be as clear cut as the above. Some people may display all overdose signs, others will have one or two.
For more signs, read our resource: How to save a life: emergency response to an overdose.
In an emergency
- Check if the person is conscious by shaking them and loudly calling their name or asking if they’re okay.
- If the person does not respond, check they are breathing.
- If there’s no response, stay calm, shout for help and call 999.
- Ask for an ambulance. Give as much information as you can and be open about what was taken – you won’t get in trouble for getting help.
- The call handler will stay on the line and talk you through what to do. If you are by yourself, put them on speakerphone to leave your hands free.
- Speak to the person, reassure them and talk them through what you are doing. They may be able to hear you even if they cannot respond.
- Administer naloxone if you have it (see naloxone guidance below).
- For people who are unresponsive and breathing, put them in the recovery position (on their side with their head tilted back) and monitor breathing.
- For people who are unresponsive and not breathing, start CPR (cardiopulmonary resuscitation – chest compressions and rescue breaths). If you have someone there, ask them to get a defibrillator.
- Stay with the person until help arrives.
Learn more about drug overdose and emergency first aid:
- Unresponsive and breathing patient (British Red Cross)
- Unresponsive and not breathing patient (British Red Cross)
- What you need to know about taking drugs (NHS inform)
- Stop The Deaths (Scottish Drugs Forum)
- Overdose (Crew)
Naloxone
Naloxone is a life-saving medicine that can temporarily reverse the effects of an opioid overdose. It will not cause the person any harm if opioids have not been used.
Although xylazine is not an opioid, naloxone should always be administered if the person is overdosing and is unresponsive. Many overdoses involve polydrug use with opioids and reversing the effects of one drug may be enough to bring the person round.
In Scotland, naloxone is available at some pharmacies and drug services. It can also be ordered online for home delivery from Scottish Families Affected by Alcohol and Drugs (SFAD).
Naloxone is very easy to administer. You can learn how to administer naloxone in a free e-learning course by the Scottish Drugs Forum (SDF).
For more information and tutorial videos, visit naloxone.org.uk (external website):
Doses should be administered one at a time, waiting 2-3 minutes between doses while watching for a response.
Be aware the person may not wake up or regain full consciousness due to the sedative effects of xylazine.
Administration should continue until:
- normal breathing is restored
- emergency services arrive and take over
- you have no naloxone left.
If multiple kits have been administered but they are having no effect, it may be that this is a different type of medical emergency. An ambulance should be called immediately, so that professional assistance can be offered as soon as possible.
Naloxone will start to wear off after 20–30 minutes. The duration of action of naloxone is shorter than that of opioid drugs, which means there is a risk of repeat overdose.
Stay with the person and monitor them. When they wake up, provide reassurance and explain who you are and what has happened.
If they go back into overdose, administer further doses of naloxone as required.
Information for people who take drugs and community members
The unregulated drug supply is increasingly toxic and unpredictable. Getting support and treatment reduces the risk of experiencing harm or dying from an overdose. Speak to your local drug service to get support. Click here to find a drug service in your area (external website).
Follow harm reduction practices
- Avoid injecting. This route of administration poses the highest risk. If you do inject, use new equipment. You can get this from your local needle exchange service. Wash your hands and injection sites (before and after).
- Know the signs of infection: heat, redness, swelling, bad smell, pain, increased size or depth or more yellow, green or black in the wound than before.
- If there are signs of infection, get medical help early to prevent further harm and injury. Call 111 for advice. Needle exchanges, GPs, minor injury clinics and pharmacies may also be able to help. In an emergency, visit the emergency department.
- Drug testing is the only way to confirm drug contents. To get a sample tested, use the free, anonymous postal service provided by WEDINOS.
- Visit wedinos.org and click sample testing.
- Print off a sample form.
- Follow the instructions to generate a reference code and make a note of the code.
- Fill in the form completely or the sample won’t be accepted.
- Put the form and drug sample (double wrapped in something leakproof) into an envelope with a stamp on it and post it to WEDINOS.
- Results will be posted online a few days later.
- Xylazine test strips are available. These can be used to show the presence of xylazine in a sample, but cannot provide information on safety, purity, quantity or other contaminants.
- Use drugs in the company of people you trust and take turns to dose.
- Tell someone what you have taken, how much and when.
- Xylazine is often mis-sold as another drug, like heroin or codeine. Take a test dose – a small amount or part of a pill.
- Always use caution, even if someone has used the batch before. The drugs may be unevenly mixed in the product.
- If someone who takes drugs regularly has stopped or cut down use, their tolerance will have reduced. This increases the risk of overdose as they will not need to take as much to get the same effect.
- Mixing drugs (including alcohol and medicines) can cause unexpected and unpredictable results and significantly increases the risk of overdose.
- As xylazine is usually found alongside other drugs, polydrug use may be unintentional. Try to minimise mixing, space out doses of different drugs, ensure you are somewhere safe and take much less than you would if you were only taking one.
- Naloxone (see above) is an effective, life-saving medicine that can temporarily reverse the effects of an opioid overdose.
- Although xylazine is not an opioid, naloxone should always be administered if the person is overdosing and is unresponsive – many overdoses involve an opioid and reversing the effects of one drug may be enough to bring the person round.
- Pick up naloxone from a drug service or order online from Scottish Families Affected by Alcohol and Drugs (SFAD).
Actions for high-risk settings
High-risk settings are places where people may take more drugs than average, often at the same time and from shared batches. Places at higher risk include prisons, hostels, supported accommodation, nightlife venues, care homes and educational settings.
People living and working in these settings should:
- Ensure their setting is prepared and ready to respond to overdose situations.
- Be vigilant to opioid use and aware of the signs of an overdose. Encourage people to report overdose signs immediately. In an emergency, stay calm and call 999.
- If appropriate, ensure people have access to hand washing facilities and clean areas to take care of wounds to prevent infection. Offer convenient and discreet access to wound care supplies, such as simple, clean and adhesive dressings (like premierpore or mepore).
- Recognise that levels of consciousness may fluctuate for several hours while under the influence. Even if the person appears alert, this may be temporary. Stay with the person and monitor closely.
- Carry and promote naloxone. Ensure the setting has multiple naloxone kits available and trained people are able to respond. Check that kits have not expired and that they are easy to access.
- Provide regular refresher training on drug-related emergencies, including information on reducing the risk of injection-related injuries, wound care, overdose, basic life support and naloxone.
Where there are concerns about exposure to substances, staff should use appropriate personal protective equipment (PPE) and follow procedures.
Actions for drug and alcohol service staff
- Services, and Alcohol and Drug Partnerships should share this alert with local partners who are likely to be in contact with people who take drugs.
- When asking patients about substance use, explain that the contents of drugs are changing and new substances like nitazenes (synthetic opioids) and xylazine are becoming more common.
- Be vigilant and proactive about asking people if they are injecting and recognise and respond proactively to high-risk injection patterns.
- Have staff members trained in assessing wounds and complications. ACT on wounds – ask, check and treat:
- Ask: Start a conversation. Explain that xylazine can cause skin damage and infections and offer a safe space to discuss wounds and wound care.
- Check: Look at sites or areas of concern. Be aware wounds can appear anywhere on the body, not just at injecting sites, and may present in people regardless of their route of administration.
- Treat: Provide convenient and discreet access to wound care supplies, such as simple, clean and adhesive dressings (like premierpore or mepore). Wounds should be treated onsite wherever possible or referred to a specialist service for treatment.
- Discuss treatment options and harm reduction approaches, including the risk of mixing drugs and the importance of drug checking.
- Service staff can help people access the drug testing service WEDINOS. Staff should not handle substances but can facilitate service access by providing printed submission forms, stamped addressed envelopes and by sharing online results.
- Xylazine test strips can be used to show the presence of xylazine in a sample, but cannot provide information on safety, purity, quantity or other contaminants.
- Xylazine can cause memory impairment. Discuss ways to keep track of appointments such as sending reminders. Make a note of key points at appointments and recap these each time you meet.
Actions for emergency service, clinical and healthcare staff
Staff working in emergency services and healthcare should be vigilant for the presentation of xylazine toxicity, particularly when working with patients who have used opioids, are not responding to naloxone, have wounds, or have low heart rate and blood pressure.
Features may be indistinguishable from concomitant opioid toxicity. Look out for:
- decreased blood pressure
- decreased consciousness
- decreased mental activity
- decreased pulse
- decreased respiration
- decreased temperature
- increased blood glucose.
The most common clinical features of patients with multi-drug toxicity including xylazine, in the ASSIST emergency department project were reduced consciousness, low heart rate and small pupils.
Be aware that testing used by clinical services is varied and new substances may not be picked up by existing urine and saliva tests. Non-detection of a drug does not mean it is not present, and a person’s clinical history is also important to determine appropriate prescribing and psychosocial interventions.
Build links with your local drug services and liaison team and in all your contacts with patients, encourage them to access support and take-home naloxone.
TOXBASE summary
- The most common features of alpha-2 receptor agonists include drowsiness, coma, bradycardia and hypotension, but signs may be indistinguishable from concomitant opioid toxicity.
- Xylazine may be associated with severe necrotic skin ulceration.
- Xylazine use is also associated with an acute withdrawal syndrome.
- The half-life in humans is around 5 hours. Sedation has been reported to last between 8 and 72 hours in overdose.
For further advice, medical professionals can use the UK National Poisons Information Service 24-hour telephone service on 0344 892 0111, or its online database, TOXBASE.
Recommendations
- The presence of xylazine as an adulterant in heroin, benzodiazepines, counterfeit pharmaceuticals and in THC vapes indicates widespread availability. Emergency care staff attending suspected incidents of drug intoxication and overdose should consider xylazine as part of their differential diagnosis.
- Xylazine has largely been identified alongside other substances including heroin and new synthetic opioids, therefore carriage and administration of naloxone remain important harm reduction measures.
- The potential for xylazine to be used as an adulterant increases the importance and need for drug checking and substance testing services, as well as routine testing within seizures.
- The highest risk of harm is associated with injection. The risk of skin and wound infections is increased with poor hygiene. This emphasises the need for safe, clean injecting spaces, and a focus on reducing injecting-related injuries.
- Scottish Government should consider how to support the scale up of wound care packages in primary care, secondary care, drug treatment and harm reduction or low threshold services as part of its urgent response to emergent substances.
Legal status
- In the UK, the supply and importation of xylazine is controlled by the Psychoactive Substances Act 2016.
- In February 2024, the Advisory Council on the Misuse of Drugs (ACMD) recommended xylazine be added to class C of the Misuse of Drugs Act 1971.
More information
- Xylazine information:
- For wound resources, visit SDF:
- For help and support or information on drugs, visit NHS inform – drugs and drug use.
- To order naloxone, visit Scottish Families Affected by Alcohol & Drugs: Take-Home Naloxone.
- Drugs giving unexpected effects? Make a report to RADAR. Use our reporting form or email drugsradar@phs.scot
